Welcome to New York Orthopaedic Spinal Associates, where we specialize in treating herniated disc disease. Our team of expert physicians, led by brothers Drs. Marc and Ira Chernoff, are dedicated to providing our patients with the highest quality care.
With over 30 years of experience and board certification in spinal care, the Chernoff brothers have built a reputation as leaders in the field. But what truly sets our practice apart is our commitment to personalized service and treating each patient like family. At New York Orthopaedic Spinal Associates, patients aren't just a number - we take the time to listen to our patients' concerns, develop individualized treatment plans, and guide them through the recovery process.
We understand that dealing with a herniated disc can be painful and disruptive, which is why our team of experts is here to help. From conservative treatments such as physical therapy and medications to advanced surgical techniques, we offer a range of options to help our patients find relief from their symptoms.
If you're suffering from a herniated disc, the top spinal specialist New York has to offer is here to help you get back to your best self. Schedule your first appointment with New York Orthopaedic Spinal Associates today.
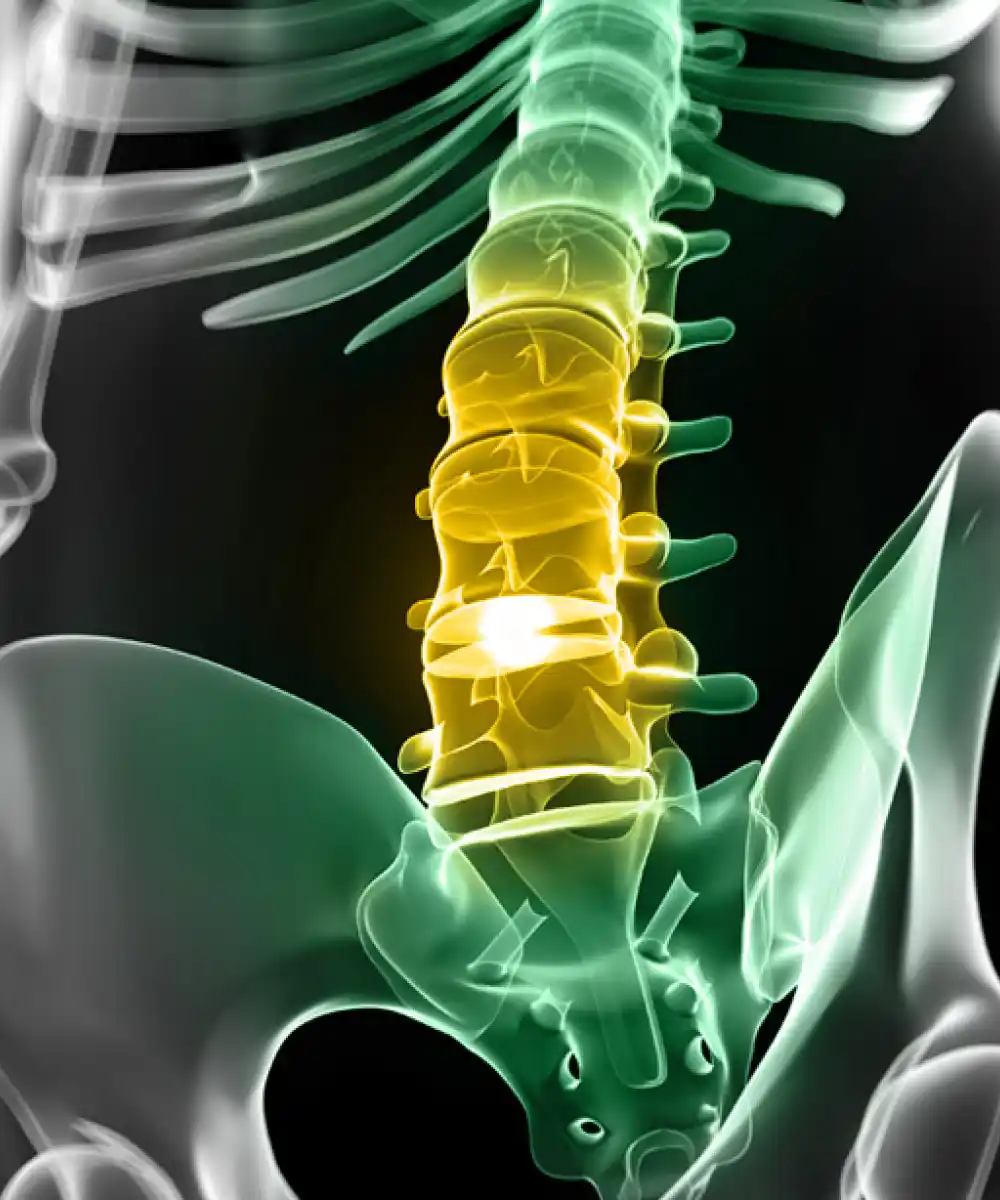
Herniated discs are some of the most common causes of neck pain and back pain. At New York Orthopaedic Spinal Associates, we specialize in diagnosing and treating herniated discs to help our patients find relief from their symptoms.
Symptoms of a herniated disc may include:
Treatment options for herniated disc disease depend on the severity of the condition, as well as the patient's individual needs and goals. Non-surgical treatments may include:
In some cases, surgery may be recommended to alleviate symptoms and restore function. Surgical options for herniated disc disease may include:
If you're experiencing symptoms of a herniated disc, the team at New York Orthopaedic Spinal Associates can help you determine the best course of treatment for your specific needs. We will work with you to develop a personalized treatment plan that helps you get back to your best self and live life to the fullest.
The most common cause of herniated disc disease is natural aging and wear and tear on the spine. However, there are other potential causes of herniated discs which include:
While these are the most common causes of herniated disc disease, there may be other factors that contribute to the condition. If you are experiencing symptoms of a herniated disc, we recommend seeking evaluation and treatment from a qualified orthopaedic specialist who can help determine the underlying causes of your symptoms and develop an appropriate treatment plan for your specific needs.
Surgery is typically not the first line of treatment for slipped or herniated discs. In most cases, conservative treatments such as physical therapy, medications, and injections can effectively manage symptoms and help patients avoid surgery.
That being said, there are situations where slipped disc surgery may be necessary. These situations include:
Yes! New York Orthopaedic Spinal Associates proudly accepts insurance from most major providers. However, we always recommend reaching out to your insurance provider and double-checking coverage before scheduling an appointment. We are happy to answer any additional questions you may have about insurance and payment options.
At New York Orthopaedic Spinal Associates, we make it as simple as possible for patients to get started on their road to recovery from spinal pain. Just request your first appointment online.